
Degenerative Disc Disease (DDD) on an MRI
Degenerative Disc Disease on MRI
Degenerative disc disease (DDD) on an MRI is common. It is worth knowing that DDD is often not the sole contributor to your pain and it may not be causing your pain at all. Back pain is the most common pain experienced by adults in America. The cause of this pain may vary from person to person, and it can also vary in severity. And, truthfully the cause can’t be identified for most. We are still learning about degenerative disc disease in many ways.
Degenerative disc disease (DDD) is a common condition that can affect individuals of nearly any age. It commonly starts in your 20’s! Treatment for DDD is available and many are diagnosed after an MRI or X-ray.
If you had an MRI and your physician told you that you have degenerative disc disease and it may be impacting your lower back pain. You may be wondering how an MRI shows degenerative changes. Today, I am going to explain degenerative disc disease and the role of MRI in diagnosing this disease. So, let’s dive in.
What is degenerative disc disease?
Degenerative disc disease (DDD) is a condition in which one or more spinal discs become compromised with age, which may cause back and neck pain.
These discs, commonly known as “shock absorbers” in the spine, are made up of strong cartilage and sit between the vertebrae in our spines. This cartilage is responsible for helping us absorb form and providing strong stable movement as we bend and rotate.
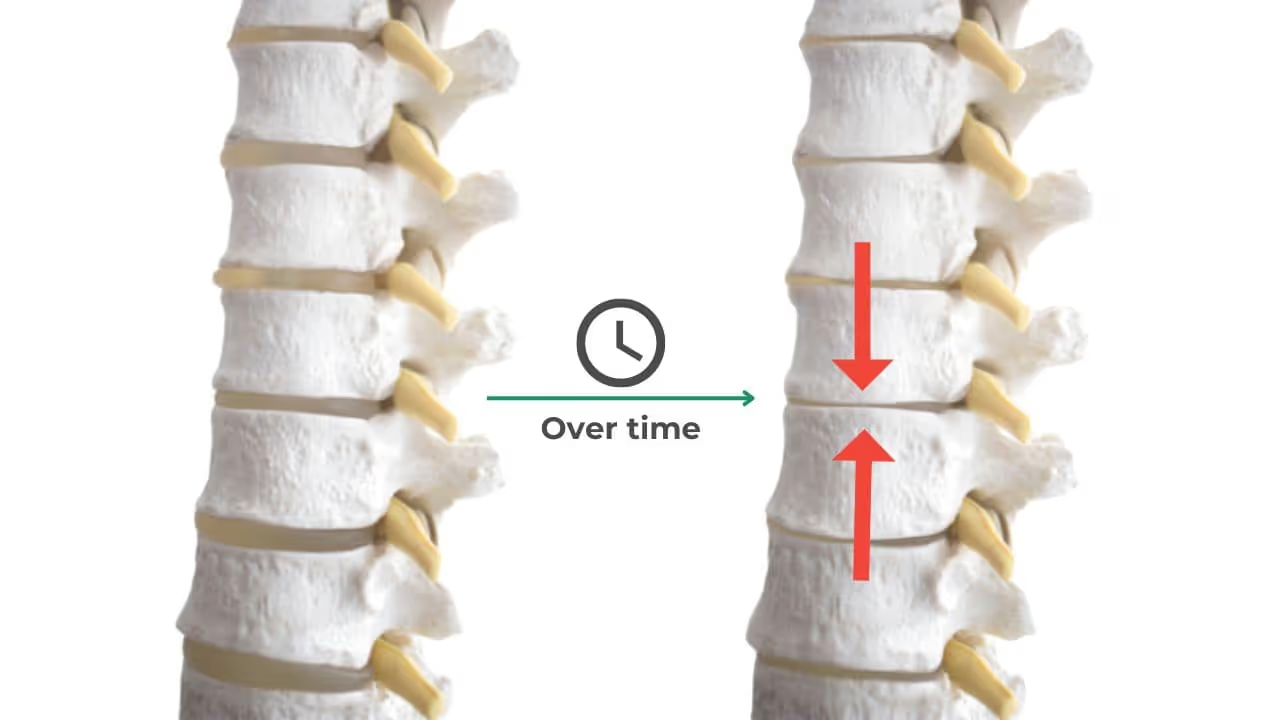
As people age, this cartilage in the spine becomes stiffer and can wear down. Stiff cartilage makes it difficult for the body to move and deteriorated discs can result in vertebrae putting pressure on other structures in your spine. All of this may cause pain, inflammation, and stiffness in the back – although some people with degenerative disc disease experience no symptoms or discomfort at all.
This is so amazing to see and the research supports that most often you don’t have pain.
When I am treating patients, I most often see people complain of stiffness. Improving back stiffness isn't as hard as it may seem.
Sometimes you can have progressive degeneration that can lead to compressed and angry nerves becoming more likely to cause pain, numbness, and muscle weakness in your legs. These symptoms down the leg are often called sciatica. In severe cases, it can also affect other body parts, such as your arms and legs. There are also different types of degenerative disc disease, based on which part of the spine is affected.
Cervical degenerative disc disease affects the top portion of the spine, known as the cervical spine. These bones are located in the neck, and if these discs begin to deteriorate, you may experience neck pain or stiffness and pain between the shoulder blades.
Thoracic degenerative disc disease affects the next section of the spine, from the bottom of the neck to the bottom of the ribcage. Thoracic discs can lead to stiffness, discomfort, or pain in your upper or mid-back.
Lumbar degenerative disc disease affects the lower back, and studies show this is the most common form of DDD. This type of degenerative disc disease can cause muscle weakness and pain in your lower back and hips. In extreme cases, pain and numbness may spread down into the legs.
You MAY need an MRI to check for spinal problems if you experience lower back pain, neck pain, numbness, tingling, and weakness in your arms and legs. The MRI may scan your whole spine or just a part of it. With that said, the need for an MRI must come from the sound judgment of your provider. There are many cases where an MRI would not be warranted and needs to be correlated with a physical exam.
An MRI, or magnetic resonance imaging, is an amazing tool for diagnosing spinal conditions because a spinal MRI can give clear, detailed pictures of your spine.
What causes degenerative disc disease?
There are multiple factors that affect an individual’s chance of developing degenerative disc disease, including
- Age
- Physical labor
- Smoking
- Lack of exercise
- Genetics
- Diet
Degenerative disc disease is a normal part of aging, but you can avoid having an advanced condition by being aware of these causes and risk factors.
Will an MRI show degenerative disc disease?
Yes, an MRI will be able to show degenerative disc disease and can give a detailed image of the condition. The MRI will show the grade of DDD, which part of the spine is being affected, and whether or not it is affecting other parts of the spine. The doctor may also use an MRI to determine if there are any other conditions that may be causing pain, such as tumors or infections. The chance of something really bad being the cause of your pain is near 1%.
MRIs are non-invasive and painless, which makes them a great diagnostic tool for degenerative disc disease. This allows the doctor to determine the best course of treatment for degenerative disc disease, and the MRI can also be used to assess whether or not surgery is necessary.
With that, we must be conscious of our healthcare spending and unnecessary testing have led not only to increased surgical rates but increased healthcare spending without a significant change in outcomes.
What are degenerative changes on MRI?
Degenerative changes on MRI are changes in the structure of the spinal cord caused by deterioration or time. You can see these changes on an MRI, and they can appear as a loss in disc height loss, a disc that is thinner than the others, a dark or black-colored disc, or a disc that bulges.
This deterioration naturally occurs as we age, but it can be worsened by repeated injury or strain, overuse of the spine, or a combination of the other factors I’ve mentioned earlier.
Degenerative changes found on an MRI may not always be DDD. Changes in the spinal cord can occur from a number of diseases and conditions, including sciatica and adult scoliosis.
What can be done to fix degenerative disc disease?
There is no cure for degenerative disc disease. That must be said. It is a natural part of aging. But, as I mentioned before, it’s often pain free. Feeling better with DDD requires a change in mindset.
Treatment for degenerative disc disease depends on the severity of the disease and typically starts with managing your pain. Your doctor may recommend medication, physical therapy, steroid injections, or a combination of these therapies. If these options do not work, surgery may be an option. Here are some of the most common treatment options available.

At Home Remedies
There are some things you can do at home to manage symptoms you have from degenerative disc disease. Making sure you rest when you have an increase in pain and using a hot pack or ice pack on the affected areas can help reduce the discomfort and pain you feel.
Most can improve on their own but utilize a movement professional to take a good look at your body and help you determine the best next step for you.

Medication
Another treatment for mild cases is an over-the-counter medication with active ingredients like ibuprofen, naproxen, or acetaminophen. These can help manage your back pain and make daily activities easier.
Muscle relaxers are also commonly used to manage back pain for those experiencing muscle spasms.
Physical Therapy
Physical therapy is used to strengthen the core muscles and improve flexibility, both of which can reduce pain and stiffness from DDD and other issues. Flexibility and strength training are common forms of physical therapy, along with massage, posture training, or using manual therapy techniques to improve pain and mobility of your spine.
Another physical therapy treatment is aquatic therapy. This is a form of physical therapy done in water to improve strength and mobility for those who may be obese or have difficulty completing land therapy.
A physical therapist will make a plan that is tailored to you and your specific medical needs. Your treatment plan may consist of one of these methods or a combination of them.
Steroid Injection
You can receive steroid injections to achieve temporary pain relief from degenerative disc disease, although there is a limit to the number of injections you can receive and they have been shown to decrease tissue integrity. There are a few types of injection treatments available.
An epidural injection uses corticosteroids to reduce the inflammation in the spine and the surrounding nerves. This is commonly used for someone with a herniated disc or nerve pain.
Nerve blockers may be used if a degenerative disc is causing nerve pain or a “pinched nerve.” A pinched nerve is caused by an excess amount of pressure on a nerve, and it can be a common symptom of degenerative disc disease. A nerve blocker involves medicine being injected into the specific affected nerve or into the nerve root. This medicine reduces inflammation surrounding the nerve and blocks pain signals from this area.
Surgery
Surgery is another option available if other treatments are not helping, if you have chronic and severe back pain, or if you have an advanced condition involving a tumor or bone fragment along the spinal cord.
There is more than one type of surgery for DDD, and the specific details of your condition determine which surgery is best for you.
A discectomy is a surgical procedure often used to treat a herniated or bulging disc. During this procedure, a doctor will remove the herniated disc and fragments that are putting pressure on your spine. An open discectomy is a more invasive procedure and requires you to stay a couple of nights at a hospital. However, a microdiscectomy is less invasive and can be done as an outpatient treatment.
Disc replacement surgery utilizes artificial discs to replace damaged ones. This surgery is typically for someone whose DDD affects only one or two spinal discs and does not affect nerves in the spine. Disc replacement surgery is also invasive, although it is ideal for maintaining mobility and flexibility in the spine and back.
Spinal fusion is another surgical option for DDD. In this procedure, a doctor will fuse two vertebrae together to become one bone. This prevents the spinal disc between the vertebrae from moving and therefore prevents pain. Unlike disc replacement surgery, spinal fusion limits mobility in the spine once the vertebrae are joined.
Exercise
Disc degeneration is a slow process, but it can be slowed and even stopped through exercise. Maintaining a regular exercise routine can strengthen back and core muscles to provide support to your spine.
There are exercises specifically designed to improve back strength, and you can adjust the difficulty level to match your abilities. You should also incorporate stretching into your daily routine. This will help you maintain a healthy back and spine.
Prevention
As with any disease or condition, prevention is key. These are my top tips for preventing degenerative disc disease:
- Stay active – get regular exercise and stretch often
- Eat an anti-inflammatory diet
- Maintain a healthy weight
- Avoid over-exerting your back or using improper form during physical activity
- Take regular movement breaks throughout your day
- Avoid smoking
It’s also a good idea to visit your primary care physician often, especially if you’re experiencing any sort of neck or back pain.
In summary,
Degenerative disc disease is a very common condition that can affect anyone but typically progresses with age. These discs wear down over time, potentially causing pain and discomfort. Injury and repeated abnormal movements can also cause discs to deteriorate faster, as well as lack of exercise, poor nutrition, and several other factors.
An MRI is a costly and non-invasive way to diagnose degenerative disc disease and to get a picture of the severity of the condition. While most of the time an MRI isn’t needed and shouldn’t be considered as first-line treatment for back pain.
If you have any lower back pain, consider seeing a movement professional because most of the time your DDD has been there for a long time and you are more recently experiencing difficulty moving.
You can also find a physical therapist to help you strengthen your core and manage any symptoms you may have.
Revision Health Services offers telehealth for Florida residents as well as massage and physical therapy locally in Jacksonville, Nocatee, and St. Johns, Florida. To find out if our services could be the best fit for you, reach out and let's chat!
Until next time, stay healthy, keep moving, and take care of yourself.
Degenerative Disc Disease on MRI
Degenerative disc disease (DDD) on an MRI is common. It is worth knowing that DDD is often not the sole contributor to your pain and it may not be causing your pain at all. Back pain is the most common pain experienced by adults in America. The cause of this pain may vary from person to person, and it can also vary in severity. And, truthfully the cause can’t be identified for most. We are still learning about degenerative disc disease in many ways.
Degenerative disc disease (DDD) is a common condition that can affect individuals of nearly any age. It commonly starts in your 20’s! Treatment for DDD is available and many are diagnosed after an MRI or X-ray.
If you had an MRI and your physician told you that you have degenerative disc disease and it may be impacting your lower back pain. You may be wondering how an MRI shows degenerative changes. Today, I am going to explain degenerative disc disease and the role of MRI in diagnosing this disease. So, let’s dive in.
What is degenerative disc disease?
Degenerative disc disease (DDD) is a condition in which one or more spinal discs become compromised with age, which may cause back and neck pain.
These discs, commonly known as “shock absorbers” in the spine, are made up of strong cartilage and sit between the vertebrae in our spines. This cartilage is responsible for helping us absorb form and providing strong stable movement as we bend and rotate.

As people age, this cartilage in the spine becomes stiffer and can wear down. Stiff cartilage makes it difficult for the body to move and deteriorated discs can result in vertebrae putting pressure on other structures in your spine. All of this may cause pain, inflammation, and stiffness in the back – although some people with degenerative disc disease experience no symptoms or discomfort at all.
This is so amazing to see and the research supports that most often you don’t have pain.
When I am treating patients, I most often see people complain of stiffness. Improving back stiffness isn't as hard as it may seem.
Sometimes you can have progressive degeneration that can lead to compressed and angry nerves becoming more likely to cause pain, numbness, and muscle weakness in your legs. These symptoms down the leg are often called sciatica. In severe cases, it can also affect other body parts, such as your arms and legs. There are also different types of degenerative disc disease, based on which part of the spine is affected.
Cervical degenerative disc disease affects the top portion of the spine, known as the cervical spine. These bones are located in the neck, and if these discs begin to deteriorate, you may experience neck pain or stiffness and pain between the shoulder blades.
Thoracic degenerative disc disease affects the next section of the spine, from the bottom of the neck to the bottom of the ribcage. Thoracic discs can lead to stiffness, discomfort, or pain in your upper or mid-back.
Lumbar degenerative disc disease affects the lower back, and studies show this is the most common form of DDD. This type of degenerative disc disease can cause muscle weakness and pain in your lower back and hips. In extreme cases, pain and numbness may spread down into the legs.
You MAY need an MRI to check for spinal problems if you experience lower back pain, neck pain, numbness, tingling, and weakness in your arms and legs. The MRI may scan your whole spine or just a part of it. With that said, the need for an MRI must come from the sound judgment of your provider. There are many cases where an MRI would not be warranted and needs to be correlated with a physical exam.
An MRI, or magnetic resonance imaging, is an amazing tool for diagnosing spinal conditions because a spinal MRI can give clear, detailed pictures of your spine.
What causes degenerative disc disease?
There are multiple factors that affect an individual’s chance of developing degenerative disc disease, including
- Age
- Physical labor
- Smoking
- Lack of exercise
- Genetics
- Diet
Degenerative disc disease is a normal part of aging, but you can avoid having an advanced condition by being aware of these causes and risk factors.
Will an MRI show degenerative disc disease?
Yes, an MRI will be able to show degenerative disc disease and can give a detailed image of the condition. The MRI will show the grade of DDD, which part of the spine is being affected, and whether or not it is affecting other parts of the spine. The doctor may also use an MRI to determine if there are any other conditions that may be causing pain, such as tumors or infections. The chance of something really bad being the cause of your pain is near 1%.
MRIs are non-invasive and painless, which makes them a great diagnostic tool for degenerative disc disease. This allows the doctor to determine the best course of treatment for degenerative disc disease, and the MRI can also be used to assess whether or not surgery is necessary.
With that, we must be conscious of our healthcare spending and unnecessary testing have led not only to increased surgical rates but increased healthcare spending without a significant change in outcomes.
What are degenerative changes on MRI?
Degenerative changes on MRI are changes in the structure of the spinal cord caused by deterioration or time. You can see these changes on an MRI, and they can appear as a loss in disc height loss, a disc that is thinner than the others, a dark or black-colored disc, or a disc that bulges.
This deterioration naturally occurs as we age, but it can be worsened by repeated injury or strain, overuse of the spine, or a combination of the other factors I’ve mentioned earlier.
Degenerative changes found on an MRI may not always be DDD. Changes in the spinal cord can occur from a number of diseases and conditions, including sciatica and adult scoliosis.
What can be done to fix degenerative disc disease?
There is no cure for degenerative disc disease. That must be said. It is a natural part of aging. But, as I mentioned before, it’s often pain free. Feeling better with DDD requires a change in mindset.
Treatment for degenerative disc disease depends on the severity of the disease and typically starts with managing your pain. Your doctor may recommend medication, physical therapy, steroid injections, or a combination of these therapies. If these options do not work, surgery may be an option. Here are some of the most common treatment options available.

At Home Remedies
There are some things you can do at home to manage symptoms you have from degenerative disc disease. Making sure you rest when you have an increase in pain and using a hot pack or ice pack on the affected areas can help reduce the discomfort and pain you feel.
Most can improve on their own but utilize a movement professional to take a good look at your body and help you determine the best next step for you.

Medication
Another treatment for mild cases is an over-the-counter medication with active ingredients like ibuprofen, naproxen, or acetaminophen. These can help manage your back pain and make daily activities easier.
Muscle relaxers are also commonly used to manage back pain for those experiencing muscle spasms.
Physical Therapy
Physical therapy is used to strengthen the core muscles and improve flexibility, both of which can reduce pain and stiffness from DDD and other issues. Flexibility and strength training are common forms of physical therapy, along with massage, posture training, or using manual therapy techniques to improve pain and mobility of your spine.
Another physical therapy treatment is aquatic therapy. This is a form of physical therapy done in water to improve strength and mobility for those who may be obese or have difficulty completing land therapy.
A physical therapist will make a plan that is tailored to you and your specific medical needs. Your treatment plan may consist of one of these methods or a combination of them.
Steroid Injection
You can receive steroid injections to achieve temporary pain relief from degenerative disc disease, although there is a limit to the number of injections you can receive and they have been shown to decrease tissue integrity. There are a few types of injection treatments available.
An epidural injection uses corticosteroids to reduce the inflammation in the spine and the surrounding nerves. This is commonly used for someone with a herniated disc or nerve pain.
Nerve blockers may be used if a degenerative disc is causing nerve pain or a “pinched nerve.” A pinched nerve is caused by an excess amount of pressure on a nerve, and it can be a common symptom of degenerative disc disease. A nerve blocker involves medicine being injected into the specific affected nerve or into the nerve root. This medicine reduces inflammation surrounding the nerve and blocks pain signals from this area.
Surgery
Surgery is another option available if other treatments are not helping, if you have chronic and severe back pain, or if you have an advanced condition involving a tumor or bone fragment along the spinal cord.
There is more than one type of surgery for DDD, and the specific details of your condition determine which surgery is best for you.
A discectomy is a surgical procedure often used to treat a herniated or bulging disc. During this procedure, a doctor will remove the herniated disc and fragments that are putting pressure on your spine. An open discectomy is a more invasive procedure and requires you to stay a couple of nights at a hospital. However, a microdiscectomy is less invasive and can be done as an outpatient treatment.
Disc replacement surgery utilizes artificial discs to replace damaged ones. This surgery is typically for someone whose DDD affects only one or two spinal discs and does not affect nerves in the spine. Disc replacement surgery is also invasive, although it is ideal for maintaining mobility and flexibility in the spine and back.
Spinal fusion is another surgical option for DDD. In this procedure, a doctor will fuse two vertebrae together to become one bone. This prevents the spinal disc between the vertebrae from moving and therefore prevents pain. Unlike disc replacement surgery, spinal fusion limits mobility in the spine once the vertebrae are joined.
Exercise
Disc degeneration is a slow process, but it can be slowed and even stopped through exercise. Maintaining a regular exercise routine can strengthen back and core muscles to provide support to your spine.
There are exercises specifically designed to improve back strength, and you can adjust the difficulty level to match your abilities. You should also incorporate stretching into your daily routine. This will help you maintain a healthy back and spine.
Prevention
As with any disease or condition, prevention is key. These are my top tips for preventing degenerative disc disease:
- Stay active – get regular exercise and stretch often
- Eat an anti-inflammatory diet
- Maintain a healthy weight
- Avoid over-exerting your back or using improper form during physical activity
- Take regular movement breaks throughout your day
- Avoid smoking
It’s also a good idea to visit your primary care physician often, especially if you’re experiencing any sort of neck or back pain.
In summary,
Degenerative disc disease is a very common condition that can affect anyone but typically progresses with age. These discs wear down over time, potentially causing pain and discomfort. Injury and repeated abnormal movements can also cause discs to deteriorate faster, as well as lack of exercise, poor nutrition, and several other factors.
An MRI is a costly and non-invasive way to diagnose degenerative disc disease and to get a picture of the severity of the condition. While most of the time an MRI isn’t needed and shouldn’t be considered as first-line treatment for back pain.
If you have any lower back pain, consider seeing a movement professional because most of the time your DDD has been there for a long time and you are more recently experiencing difficulty moving.
You can also find a physical therapist to help you strengthen your core and manage any symptoms you may have.
Revision Health Services offers telehealth for Florida residents as well as massage and physical therapy locally in Jacksonville, Nocatee, and St. Johns, Florida. To find out if our services could be the best fit for you, reach out and let's chat!
Until next time, stay healthy, keep moving, and take care of yourself.
References:
1. Suthar P, Patel R, Mehta C, Patel N. MRI evaluation of lumbar disc degenerative disease. J Clin Diagn Res. 2015 Apr;9(4):TC04-9. doi: 10.7860/JCDR/2015/11927.5761. Epub 2015 Apr 1. PMID: 26023617; PMCID: PMC4437133
2. Kos N, Gradisnik L, Velnar T. A Brief Review of the Degenerative Intervertebral Disc Disease. Med Arch. 2019 Dec;73(6):421-424. doi: 10.5455/medarh.2019.73.421-424. PMID: 32082013; PMCID: PMC7007629.





.jpg)
