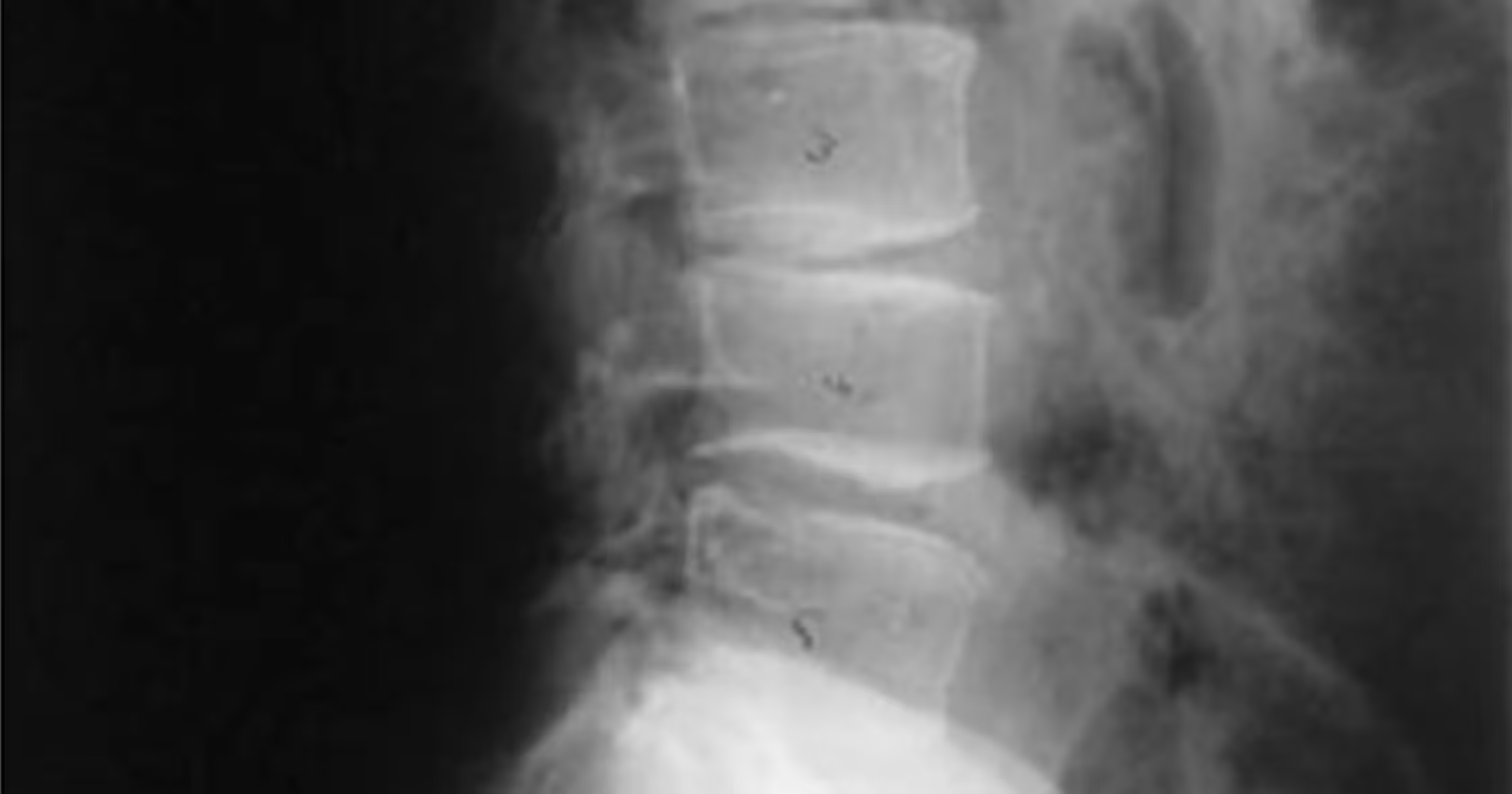
What I Tell My Patients To Avoid With Degenerative Disc Disease?
Things to avoid with degenerative disc disease include advanced imaging such as MRIs and not remaining active. Let me explain why this is so important!
To understand what things you should avoid with degenerative disc disease it is worth gaining a little better understanding of degenerative disc disease.
What Is degenerative disc disease (DDD)?
Degenerative disc disease is a common condition in which the intervertebral disc losses height and changes its composition. This composition change can include a loss of water and elastic properties. Essentially, the disc becomes less mobile and a little stiffer. It is not appropriate to call disc degeneration a disease. It is a normal part of aging. I said, NORMAL! It's equivalent to saying wrinkles are a disease on your skin. We must understand that degenerative disc disease is normal. If we do this, we can better manage it and have fewer limitations from it.
It has been shown that people with progressive and severe degenerative disc disease can have a lot of discomforts or a little.
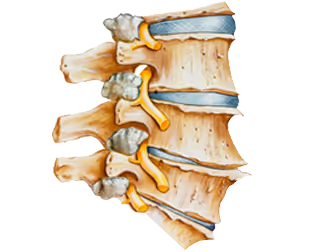
Pain from degenerative disc disease is very inconsistent. It has been shown that people with progressive and severe degenerative disc disease can have a lot of discomforts or a little. This can make some feel a little anxious because we want to know what is causing our pain. This can lead us to want an MRI but most often imaging isn't appropriate for back pain. Most people with degenerative disc disease don't have pain.
What is a Disc?
An intervertebral disc or disc is the shock absorber of the spine. They live in the entire spine and are very resilient. They are small structures with a firm outer layer and a soft gelatinous inner layer that's mostly water. They flex, pull, and twist with you as you move about your day. They are strong but as you will see, they are prone to aging and other factors, just like the rest of your body.
Just like tires on a car, a normal disc shows wear and tear over time. Intervertebral discs rely on movement to move fluid and healing factors in and out even if there is some damage or degeneration over time. This can help explain why some feel stiff after not moving and feel better once they start moving. This is common and often a good thing. I say good because motion is lotion and I would much rather see someone be able to rely on movement for relief rather than medication.
In my opinion, pain related to degenerative disc disease comes from two things. Chemical changes and mechanical changes.
- Chemical changes include inflammation systemically and locally. Systemically from other conditions such as diabetes, heart disease, poor diets, etc. Locally from the inflammation from the disc material or local joints.
- Mechanical changes can include age-related changes in surrounding joints such as osteoarthritis and facet degeneration as well as weight management and related muscular strength.
That's why when I treat degenerative disc disease we may need a more holistic approach to addressing your pain and limitations. We look at the body as a whole, not as a body part. Inflammation management may have a stronger role than we think. We can't focus on structural changes such as disc height loss and other normal findings, we need to focus on how you feel and how resilient are you when it comes to lower back pain.
Top 2 things to avoid with degenerative disc disease
If you have degenerative disc disease avoiding advanced imaging and sedentary lifestyles can help you from feeling worse and receiving unnecessary treatment. When I treat patients with degenerative disc disease we often start by reviewing the need for imaging and education on exercise.
Advanced imaging
It's been shown that receiving advanced imaging without the proper education can lead to unnecessary treatments such as medication and surgery. For example, you go to the doctor with lower back pain. They order an MRI and those results are then uploaded to your patient portal. You read your results and start Googling. That can lead you down some paths you don't want to go. In contrast, if you do receive imaging then the ordering provider should sit down and review it with you. They should review how the findings of the MRI correlate to your symptoms and what the best evidence says you should do next. This would be a better experience for everyone and save thousands of healthcare dollars.
Sedentary lifestyle; Stop moving and exercising
Our body, especially the joints and structures impacted by degenerative disc disease, crave movement. Nearly all of my patients report relief when they are moving. Not only can exercise reduce symptoms of DDD such as stiffness and pain but it can help you reduce your long-term pain and disability. How you exercise and how much is different for everyone but I highly recommend that you give your body the gift of time with a movement specialist to receive a good examination and learn how to exercise safely so you can not only feel better now but for years to come.
How do I stop degenerative disc disease from progressing?
The progression of degenerative disc disease is inevitable. Nearly every human being on this earth will have degenerative disc disease to some extent. You can assume that as you get older you will have more and more degeneration, on an image such as an MRI. Degeneration is very normal because we are not built to last forever. The good news is that it doesn't mean you will have pain! That's right, pain can be independent of the amount of degeneration. How you feel can always improve. Let's explore what a disc is and the treatments for degenerative disc disease.
What are the causes of degenerative disc disease?
It is generally understood that degenerative disc disease is caused by time. Honestly, it is a part of aging or due to the wear and tear from everyday activities. This is good, we want to become older active adults. Occasionally, a severe injury resulting in a major herniation early in life can lead to early degenerative disc disease. Generally, we associate degenerative disc disease with common risk factors including:
- Increase time sitting
- Obesity
- Smoking
- Heavy physical labor for long periods of time
- Genetics (not as likely as environmental/physical factors, such as activity and lifestyle choices.
Degenerative changes generally start in one's early 20s but rarely cause symptoms.
Degenerative changes generally start in one's early 20s but rarely cause symptoms. Crazy right??? Once we reach our 60s, most people have some form of degenerative disc changes and most don't have any symptoms! Many people with degenerative disc disease are asymptomatic and it is only discovered after imaging is done for an unrelated issue.
How Is Degenerative Disc Disease Diagnosed?
Diagnosis generally occurs after an examination by your physician or physical therapist based on your signs and symptoms. Imaging may also be used to diagnose degenerative disc disease. These include CT scans, X-rays, and MRIs. Nearly 100% of the time, it is not an independent diagnosis. That means, it is also seen with other age-related conditions such as facet arthropathy, disc herniations, and bulges.
However, it is recommended that imaging results be used with caution. Multiple studies have shown that pathology (findings on an MRI) does NOT equal pain. What appears on an image is rarely the cause of one's symptoms. Studies also show that receiving imaging leads to an increased likelihood of unnecessary surgical intervention.
Best treatments for degenerative disc disease
Degenerative disc disease should be treated conservatively. This means when you have degenerative disc disease the first step should be to stay away from imaging and surgery.
5 top ways to treat degenerative disc disease include education, mindset, exercise, movement, and building your team.
1. Education
We know that degenerative disc disease is very common and oftentimes not painful. It would be worth learning more about your body and the factors contributing to pain vs. trying to find the exact cause.
2. Mindset
You can get better and have pain relief. You just need to believe it though. It will take some time and resources but it can be managed.
3. Exercise
Exercise is the best long-term management for degenerative disc disease. Yes, I am biased but there is also a lot of high-level evidence to support this. The type of exercise, the amount, and other specifics are unique to every person but once you find what works for your body not only can your pain decrease but you can do more with less discomfort. A win-win!
I recommend a good physical exam with a movement expert such as a physical therapist can help you dial in a perfect program and routine for you! I have seen many people get better and stay better after a course of physical therapy. This is a self paced course I put together to help people hit all of these bullet points.
If you are in Nocatee, Florida or the surrounding area reach out and we can discuss a plan that will help you feel better!
4. Movement
A good mobility program to improve how your joint movement can be key. It is not uncommon to have stiffness associated with degenerative disc disease. Mobility can improve this stiffness and a few minutes every day can help feel better and manage without medication.
5. Build your team
Degenerative disc disease is not technically curable but it is manageable. You can absolulty have no pain with disc degeneration. I have seen it many times. Most people can manage with exercise, modalities such as heat, ice, and intermittent medication. For those with chronic back pain I do recommend that you start building your team so you can have people to lean on during the acute flare ups. I recommend having a good massage therapist, physical therapist, and primary care provider that will help you conservatively manage your discomfort. If you are in the Jacksonville area, I know great providers that can absolutely help you out!
In summary, we reviewed many aspects of degenerative disc disease ranging from what to avoid, the best evidence, and ways you can feel better. As a system, we need to normalize common findings on MRIs such as degenerative disc disease. It's okay that we develop this. In the same breath, you can absolutely feel better and don't have pain. There are many options to improve how your pain and what you can do. Team up with a physical therapist so you can learn about your body and discover how to be successful today and for years to come.
Revision Health Services now offers Telehealth for Florida residents as well as massage and physical therapy locally in Jacksonville, Nocatee, and St. Johns, Florida. To find out if our services could be the best fit for you, reach out and let's chat!
Until next time, stay healthy, keep moving, and take care of yourself.
Things to avoid with degenerative disc disease include advanced imaging such as MRIs and not remaining active. Let me explain why this is so important!
To understand what things you should avoid with degenerative disc disease it is worth gaining a little better understanding of degenerative disc disease.
What Is degenerative disc disease (DDD)?
Degenerative disc disease is a common condition in which the intervertebral disc losses height and changes its composition. This composition change can include a loss of water and elastic properties. Essentially, the disc becomes less mobile and a little stiffer. It is not appropriate to call disc degeneration a disease. It is a normal part of aging. I said, NORMAL! It's equivalent to saying wrinkles are a disease on your skin. We must understand that degenerative disc disease is normal. If we do this, we can better manage it and have fewer limitations from it.
It has been shown that people with progressive and severe degenerative disc disease can have a lot of discomforts or a little.

Pain from degenerative disc disease is very inconsistent. It has been shown that people with progressive and severe degenerative disc disease can have a lot of discomforts or a little. This can make some feel a little anxious because we want to know what is causing our pain. This can lead us to want an MRI but most often imaging isn't appropriate for back pain. Most people with degenerative disc disease don't have pain.
What is a Disc?
An intervertebral disc or disc is the shock absorber of the spine. They live in the entire spine and are very resilient. They are small structures with a firm outer layer and a soft gelatinous inner layer that's mostly water. They flex, pull, and twist with you as you move about your day. They are strong but as you will see, they are prone to aging and other factors, just like the rest of your body.
Just like tires on a car, a normal disc shows wear and tear over time. Intervertebral discs rely on movement to move fluid and healing factors in and out even if there is some damage or degeneration over time. This can help explain why some feel stiff after not moving and feel better once they start moving. This is common and often a good thing. I say good because motion is lotion and I would much rather see someone be able to rely on movement for relief rather than medication.
In my opinion, pain related to degenerative disc disease comes from two things. Chemical changes and mechanical changes.
- Chemical changes include inflammation systemically and locally. Systemically from other conditions such as diabetes, heart disease, poor diets, etc. Locally from the inflammation from the disc material or local joints.
- Mechanical changes can include age-related changes in surrounding joints such as osteoarthritis and facet degeneration as well as weight management and related muscular strength.
That's why when I treat degenerative disc disease we may need a more holistic approach to addressing your pain and limitations. We look at the body as a whole, not as a body part. Inflammation management may have a stronger role than we think. We can't focus on structural changes such as disc height loss and other normal findings, we need to focus on how you feel and how resilient are you when it comes to lower back pain.
Top 2 things to avoid with degenerative disc disease
If you have degenerative disc disease avoiding advanced imaging and sedentary lifestyles can help you from feeling worse and receiving unnecessary treatment. When I treat patients with degenerative disc disease we often start by reviewing the need for imaging and education on exercise.
Advanced imaging
It's been shown that receiving advanced imaging without the proper education can lead to unnecessary treatments such as medication and surgery. For example, you go to the doctor with lower back pain. They order an MRI and those results are then uploaded to your patient portal. You read your results and start Googling. That can lead you down some paths you don't want to go. In contrast, if you do receive imaging then the ordering provider should sit down and review it with you. They should review how the findings of the MRI correlate to your symptoms and what the best evidence says you should do next. This would be a better experience for everyone and save thousands of healthcare dollars.
Sedentary lifestyle; Stop moving and exercising
Our body, especially the joints and structures impacted by degenerative disc disease, crave movement. Nearly all of my patients report relief when they are moving. Not only can exercise reduce symptoms of DDD such as stiffness and pain but it can help you reduce your long-term pain and disability. How you exercise and how much is different for everyone but I highly recommend that you give your body the gift of time with a movement specialist to receive a good examination and learn how to exercise safely so you can not only feel better now but for years to come.
How do I stop degenerative disc disease from progressing?
The progression of degenerative disc disease is inevitable. Nearly every human being on this earth will have degenerative disc disease to some extent. You can assume that as you get older you will have more and more degeneration, on an image such as an MRI. Degeneration is very normal because we are not built to last forever. The good news is that it doesn't mean you will have pain! That's right, pain can be independent of the amount of degeneration. How you feel can always improve. Let's explore what a disc is and the treatments for degenerative disc disease.
What are the causes of degenerative disc disease?
It is generally understood that degenerative disc disease is caused by time. Honestly, it is a part of aging or due to the wear and tear from everyday activities. This is good, we want to become older active adults. Occasionally, a severe injury resulting in a major herniation early in life can lead to early degenerative disc disease. Generally, we associate degenerative disc disease with common risk factors including:
- Increase time sitting
- Obesity
- Smoking
- Heavy physical labor for long periods of time
- Genetics (not as likely as environmental/physical factors, such as activity and lifestyle choices.
Degenerative changes generally start in one's early 20s but rarely cause symptoms.
Degenerative changes generally start in one's early 20s but rarely cause symptoms. Crazy right??? Once we reach our 60s, most people have some form of degenerative disc changes and most don't have any symptoms! Many people with degenerative disc disease are asymptomatic and it is only discovered after imaging is done for an unrelated issue.
How Is Degenerative Disc Disease Diagnosed?
Diagnosis generally occurs after an examination by your physician or physical therapist based on your signs and symptoms. Imaging may also be used to diagnose degenerative disc disease. These include CT scans, X-rays, and MRIs. Nearly 100% of the time, it is not an independent diagnosis. That means, it is also seen with other age-related conditions such as facet arthropathy, disc herniations, and bulges.
However, it is recommended that imaging results be used with caution. Multiple studies have shown that pathology (findings on an MRI) does NOT equal pain. What appears on an image is rarely the cause of one's symptoms. Studies also show that receiving imaging leads to an increased likelihood of unnecessary surgical intervention.
Best treatments for degenerative disc disease
Degenerative disc disease should be treated conservatively. This means when you have degenerative disc disease the first step should be to stay away from imaging and surgery.
5 top ways to treat degenerative disc disease include education, mindset, exercise, movement, and building your team.
1. Education
We know that degenerative disc disease is very common and oftentimes not painful. It would be worth learning more about your body and the factors contributing to pain vs. trying to find the exact cause.
2. Mindset
You can get better and have pain relief. You just need to believe it though. It will take some time and resources but it can be managed.
3. Exercise
Exercise is the best long-term management for degenerative disc disease. Yes, I am biased but there is also a lot of high-level evidence to support this. The type of exercise, the amount, and other specifics are unique to every person but once you find what works for your body not only can your pain decrease but you can do more with less discomfort. A win-win!
I recommend a good physical exam with a movement expert such as a physical therapist can help you dial in a perfect program and routine for you! I have seen many people get better and stay better after a course of physical therapy. This is a self paced course I put together to help people hit all of these bullet points.
If you are in Nocatee, Florida or the surrounding area reach out and we can discuss a plan that will help you feel better!
4. Movement
A good mobility program to improve how your joint movement can be key. It is not uncommon to have stiffness associated with degenerative disc disease. Mobility can improve this stiffness and a few minutes every day can help feel better and manage without medication.
5. Build your team
Degenerative disc disease is not technically curable but it is manageable. You can absolulty have no pain with disc degeneration. I have seen it many times. Most people can manage with exercise, modalities such as heat, ice, and intermittent medication. For those with chronic back pain I do recommend that you start building your team so you can have people to lean on during the acute flare ups. I recommend having a good massage therapist, physical therapist, and primary care provider that will help you conservatively manage your discomfort. If you are in the Jacksonville area, I know great providers that can absolutely help you out!
In summary, we reviewed many aspects of degenerative disc disease ranging from what to avoid, the best evidence, and ways you can feel better. As a system, we need to normalize common findings on MRIs such as degenerative disc disease. It's okay that we develop this. In the same breath, you can absolutely feel better and don't have pain. There are many options to improve how your pain and what you can do. Team up with a physical therapist so you can learn about your body and discover how to be successful today and for years to come.
Revision Health Services now offers Telehealth for Florida residents as well as massage and physical therapy locally in Jacksonville, Nocatee, and St. Johns, Florida. To find out if our services could be the best fit for you, reach out and let's chat!
Until next time, stay healthy, keep moving, and take care of yourself.
1. Chou R, Fu R, Carrino JA, Deyo RA. Imaging strategies for low-back pain: systematic review and meta-analysis. Lancet. 2009 Feb 7;373(9662):463-72. doi: 10.1016/S0140-6736(09)60172-0. PMID: 19200918. 2. Kos N, Gradisnik L, Velnar T. A Brief Review of the Degenerative Intervertebral Disc Disease. Med Arch. 2019 Dec;73(6):421-424. doi: 10.5455/medarh.2019.73.421-424. PMID: 32082013; PMCID: PMC7007629. 3. Brinjikji W, Luetmer PH, Comstock B, Bresnahan BW, Chen LE, Deyo RA, Halabi S, Turner JA, Avins AL, James K, Wald JT, Kallmes DF, Jarvik JG. Systematic literature review of imaging features of spinal degeneration in asymptomatic populations. AJNR Am J Neuroradiol. 2015 Apr;36(4):811-6. doi: 10.3174/ajnr.A4173. Epub 2014 Nov 27. PMID: 25430861; PMCID: PMC4464797.
2. Donnally III CJ, Hanna A, Varacallo M. Lumbar Degenerative Disk Disease. [Updated 2022 Sep 4]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK448134/

.jpg)
.jpg)

